Drugs for Life
- Joseph Dumit, PhD
- Assistant Professor of Anthropology and Science & Technology Studies at MIT. E-mail dumit{at}mit.edu; fax 617-258-8118.
If you happen to have a serotonin imbalance in your brain…ssri’s [SSRI, selective serotonin reuptake inhibitor] can change
that. …[T]hat I have to take some pills every day to maintain my life is no different from my friend who takes sulfa drugs
daily to stave off a recurrence of colitis, or another who injects herself with insulin.
—patient on antidepressant medication
I think being on five or more drugs for life is a minimum! Based on the latest clinical trials, almost everyone over thirty
should be on cholesterol-lowering drugs.
—MD-PhD in discussion at a neuroethics conference
For the two people quoted above (1), being on drugs for life is a normal condition: drugs should be prescribed to maintain life under certain suboptimal health conditions; drugs lengthen and improve life; and drugs are needed lifelong. These three meanings have converged around a pharmaceutical worldview in the U.S. over the past ten years and form the basis for a new paradigm of health, illness, treatment, and normalcy.
In order to make this paradigm explicit, I will draw from the philosopher and naturalist Aristotle. Aristotle was an astute observer of the world and people in it. Even in his Physics, he paid as much attention to how his fellow humans spoke about the world as to the phenomena themselves. In these activities he was a kind of cultural anthropologist of his own society.
The concept of “cause” in particular occupied Aristotle because of its variety. “Causes are spoken of in many ways,” he opined, “and there are many causes of the same thing, too.” By the latter phrase, he does not have in mind multiple causation, but the different ways in which people ascribe causes to something. Aristotle outlines four distinct kinds of causes that people use together to talk about a wooden chair. The first two he calls “contributory causes;” these are the formal cause, and the material cause. The formal cause of a chair is the form or ideal that leads to the chair being made in a certain way. This could be a model chair, or the idea of the chair in the mind of the craftsman. The material cause of the chair is the wood that is the cause of the chair’s physicality or existence.
The other two kinds of causes Aristotle calls “causes in the strict sense.” These are the efficient cause and the final cause. The efficient cause of the chair is the craftsman as the source of change that leads to the chair. The final cause of something is the use or purpose for which the thing comes about. The final cause of the chair is the need for something to sit on.
This discussion might seem a bit abstract and remote for molecular interventions, but as a medical anthropologist, I would like to suggest that contemporary U.S. ways of talking about illnesses in the context of pharmaceuticals is shifting from one causal worldview to another. If I may be allowed to simplify first and later complicate the issue, a major twentieth-century way of talking about illnesses was the bacterial-disease model. In this paradigm or worldview, an infectious agent (e.g., a bacterium or virus) was understood as the efficient cause, which caused a change in the material of an inherently healthy body. The form of illness was a disease course: the agent attacks; the healthy body fights the agent, causing symptoms; and sometimes with the help of modern medicine, the healthy body defeats the agent and returns to normal. The final cause of illness here is thus health. It may at first seem strange to talk about the purpose of an illness, but remember that we are interested in how people talk about it. If someone asked, “Why did I get sick?” one of the answers a doctor would give might be, “You are experiencing your illness because your body is fighting something bad in order to make you healthy once again.” The body is understood here as a robust system whose normal destiny is to return to health. There are many variations on this theme; even cancer and immune diseases have tended to be talked about as sustained assaults on the body (even tricking the body to fight itself), with medicine working as an ally with the robust body to return the individual to health.
This traditional paradigm is one of “inherent health,” as it assumes that most people are healthy at their core, and that most illnesses are temporary interruptions in their lives. Chronic diseases, like diabetes, cystic fibrosis, and Huntington’s, although well-known for centuries, were exceptions to the basic paradigm of inherent health. In the 1990s and into the twenty-first century, a very different notion of illness has taken center stage, one in which bodies are “inherently ill.” Diabetes and Huntington’s disease are today regularly invoked together as paradigmatic templates for almost all conditions. The older notion is not gone, of course; it coexists, and we are quite good at code-switching between both views. But this new notion of illness is one that is now promoted to us in advertisements and in awareness campaigns throughout our daily life.
The point of isolating and describing this paradigm in contrast to a previous one is not to make them equal, or to suggest that the current one is wrong. In terms of a biomedical understanding of many syndromes today, especially the mental illnesses, I think that the new paradigm is scientifically more accurate. As a medical anthropologist who studies how people talk about and understand their illnesses, I am interested in how this new paradigm of an “inherently ill” body comes to be learned and seen as natural, and what sorts of consequences it has for our understanding of what is normal and for the role of pharmaceuticals in our life.
Depression Curve
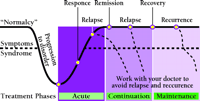
The key symbol of this new paradigm of illness is provided by the Kupfer curve as illustrated on a number of antidepressant Web sites (2). This chart (see Figure 1) tells a story about depression, its course, and treatment. But it also assumes and reinforces a more basic story about disease and health, one that has far-reaching consequences for how we, as scientists and lay people, imagine drugs and normality.
The labels on the chart define categories of health relationally. The first set is perhaps the most significant: “normalcy,” symptoms, and syndrome. The line between symptoms and syndrome is just that—a dotted line. One extra symptom, it implies, and you cross over into the syndrome, in this case into depression. Normalcy is in quotation marks, as if it were not an actual state but an ideal one. It presumably refers to a state of very few symptoms.
This image of symptoms adding up to a syndrome is of course standardized in both the Diagnostic and Statistical Manual of Mental Disrders and in the ubiquitous surveys that one finds on the Web, in mental health awareness brochures, in advertisements, and in doctors’ offices. The surveys are usually based on self-assessment of one’s own everyday symptoms—everyday in the sense that each symptom is quite common, and the only question is how often such a symptom occurs. For instance, the Zung assessment tool for depression includes statements like, “I feel downhearted, blue, and sad” and “morning is when I feel best,” both of which one answers by selecting from among “not often,” “sometimes,” “more often,” and “all the time” (3).
A weighted algorithm, or simple adding up of symptoms, is then performed to realize a score that can be enough to suggest
that one has passed into the syndrome state. In most of these surveys, no person is symptom-free. Therefore, in terms of the
iconography of the curve, one is always progressing toward the disorder. The consequences are apparent in terms of a concept
or logic of health: First, the normal state is one of vulnerability and precariousness, requiring a constant vigilance for
further warning signs. Second, the area just above the syndrome line is a kind of risk-territory and is worth defining as
a penumbra of the disorder, a kind of proto-disorder. Peter Kramer calls this process “diagnostic creep.” The third consequence
is that any shift in the line has profound personal and social consequences. On a personal level, it shifts a large number
of people into or out of “really” being ill. Socially, it shifts these people into or out of official diagnostic categories,
with big market consequences for medications, as indicated by a marketing brochure aimed at clients with interests in promoting
pharmaceuticals (4):By now you’ve seen the barrage of commercials starring good-looking people tripping over themselves or doing belly flops into
pools because they have high cholesterol. Why all the commotion? Well back in May 2001, the [National Cholesterol Education
Program (of the NIH)] changed its guidelines for the first time in ten years regarding detection, evaluation, and treatment
of heart disease. For those of you with products to sell, these guidelines essentially tripled the market for the number of
people who should be on drugs or some kind of lifestyle therapy by lowering the risk range of cholesterol.
Returning to the curve (Figure 1), the purple areas refer to treatment, in this case with an antidepressant. In the best case, one returns to “normalcy” using the medication. Treatment is not inscribed as a cure here. Rather, a series of dotted lines represent the dangers of going off the medication at any time. Diabetes is often proffered to patients as an example of the importance of staying on medication even if one feels better. Even though there are suggestions in the text of label inserts that some people are able to discontinue their medication after six to twelve months, the implication of the final phase, “maintenance,” is that depression is not like a bacterial infection, cured by a week of antibiotics. It is a lifelong condition that can be maintained at acceptable levels through lifelong pharmaceuticals: The new “normalcy” is thus not a return to the previous set of symptoms, but a “virtual” normalcy that is dependent upon medication.
Factoring in Risk
An episode of depression is thus both a condition to be treated and a prediction of future episodes. This way of talking is
made explicit in a report by Boston Life Sciences for a brainscan diagnostic test for Attention Deficit Hyperactivity Disorder:Half of all children diagnosed with ADHD continue to manifest symptoms throughout their adult life.
A diagnosis of ADHD thus also functions as a prediction, namely, that the individual is likely never to be cured. A diagnosed symptom is thus also a risk factor for chronic illness. Building on the notion of genetic risk factors, where correlation is often talked about popularly as causation, a diagnosis of depression or ADHD indicates an inherent illness. This implication is spelled out later in the same report that half of children diagnosed with ADHD will require medication for life:
Studies show that 90% of school-aged patients improve on stimulant medication, 80% continue using the medications as teenagers,
and 50% require medication throughout adulthood.
As the depression curve implies and these statements make clear, the transition from “remission” to “recovery” is a fraught one. The recovered individual is at risk for future recurrences by virtue of the fact that he or she has attained syndrome status in the past. This risk, moreover, can indicate medication as much as the actual syndrome does. As shown in Box 1, we can thus arrive at an image of the mentally ill individual body in neuroscience by either of two ways.
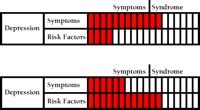
Symptoms and/or Risk Factors Add up to a Syndrome
The top bar represents the phenotype or symptom expression as measured by surveys, diagnostic tests, the DSM, etc. The bottom bar represents the total risk factor analysis. In this image, if either bar crosses the syndrome line, treatment is indicated.
The risk factor bar crossing the syndrome line is what is pointed at with the notion of maintenance or preventative therapy (whether prophylactic mastectomy or an SSRI). These charts are like meters that one should keep an eye on. In mental illness, the analogy is clearly that of neurochemical imbalances getting too great. Just as one’s symptoms cross the line, so too does one’s serotonin. The logic of these descriptions evokes what might be called the “Pharmaceutical Self,” an individual whose everyday experience of his symptoms is as if he is on bad drugs, too little serotonin perhaps, and in need of good drugs, like an SSRI, to balance the bad one out and bring both biochemistry and symptoms to proper levels.
This paradigm of diseases goes beyond mental illnesses, of course. The average middle-aged American is faced with a wide array of tests and surveys to pay attention to: cholesterol levels, prostate-specific antigen tests, breast cancer genetic screens, etc. Each of these is defined by threshold numbers that in advertisements and educational materials are promoted as more important than weight, strength, or breast size. Each threshold, once crossed, suggests strongly that one should take action and start treatment to help manage that threshold. The thresholds may be determined differently by various contingencies of the health care community, and a process of regulatory arbitration may ultimately determine who is “ill” and who is not.
Pharmaceutical Normalcy
In the “inherent illness” paradigm, most syndromes, like depression and ADHD, are understood as quite different causally from the “inherently healthy” paradigm. In the logic I have been describing, the material cause of a depressed person is their brain or phenotype, and the formal cause is their genotype. The brain serves to answer where the illness is and how it and the rest of the person’s mind subsists. Depression is said to be “in the brain,” but not “in the serotonin” (even if correcting the serotonin imbalance stops the depression). Our genes are talked about as the formal cause of our syndromes in general, informing who we will become.
Material or formal kinds of causes (e.g., one’s brain or one’s genes) applied to discussions of disease and therapeutics are not surprising, but they are worth noting because they seem so obvious today. They also serve as rhetorical barriers to other potential candidates, such as society, the environment, and family, that can be designated as indirect or secondary causes that help to shape the brain or to modify genetic programs that in turn primarily cause the illness. For example, in a Newsweek article, “Why the Young Kill,” Sharon Begley reports on the causes of violence as follows:
Brain scans show why not every child who has access to guns kills…Nothing in itself is a cause, but with a “vulnerable baby,” environment, parenting, and
stress can cause a neglected kid to emerge. The neglected kid then seizes on cultural scripts.
In this discourse, the environment is referred to as a kind of trigger: environment and society act on the abnormal “vulnerable” brain that is but a product of a genetic program. Referring to the environment as a kind of trigger reinforces the sense that the real or proximate cause is the neurochemistry that is already predisposed toward the problem, waiting to be triggered. The triggers here are portrayed as non-negotiable; what is manageable is biochemistry.
The Aristotelian final cause of one’s symptoms here is one’s body as chronically ill. Bertram Russell said of the final cause, “The nature of an acorn is to become an oak tree.” Today we often talk about how we need to prevent a person with X gene and Y brain from becoming ill, as if they are destined to that illness, as if it is inherent in their body the way an oak tree is inherent in an acorn. In this way we have re-described the core of depression from being episodes to the episodes manifesting the underlying chronic illness. What is quite unique in this view is that, because each person has their own specific genotype, phenotype, and life risk factors, each person has their own combination of inherent illnesses. This notion of the chronically ill body as final cause is also in accord with illness identity politics in which shared syndromes are seen as shared nature, shared identity, and shared destiny (5).
Lastly, the efficient cause of one’s mental state is the biochemical imbalance crossing the threshold from symptoms to syndrome. Interrupting this process is the aim of pharmacological interventions. Many pharmaceutical ads provide succinct illustrations of this “inherently ill” paradigm, touching on all four types of causes (6):
Research has shown that depression and anxiety disorders could be linked to a chemical imbalance in the brain. A family history
of these conditions might also play a role in their development.…Depression and anxiety disorders usually require long-term
treatment because of their chronic (ongoing) nature and the risk of relapse. So, even if you begin to feel better, [medicaion]
is important to take … for as long as your doctor advises. You should not stop … unless your doctor tells you it is all right to do so.
Together, the four causes presented in Table 1 constitute both a necessary and a sufficient logic of health today. They define the nature of problems as a body that is destined to become ill; the past as genetic dispositions which can be identified; the present location within imbalances; and the future as an ongoing negotiation with therapy that returns and maintains the body within normal tolerance.
The Four Causes of Mental Illness under Neurogenetic Logic
The entailments of this causal logic are fascinating. First, health is no longer homeostatic. Medical historian Georges Canguilhem has described how pathology is viewed according to its own norms. We have bodies whose destiny is pathology. Patients tend toward a disease state given their genes, and they stay in that state once they get there, according to their bodies and brains. The image of the depression curve is quite apt here: one is only precariously in the “normal state.” The question is not really whether one will slide down into syndrome, but when.
As I indicated before, this paradigm is itself not new: diabetics, biologists, and doctors have known it for a long time. But the reconfiguration of virtually all apathogenic conditions as chronic is new. The result is a notion of dependent normality, alongside the notion that it is normal to be destined to be dependent (7). I’ll conclude with a comment from one layperson helping another understand this logic:
The SSRI’s are actually not more effective in treating depression than many of the older antidepressant drugs, but they are
much safer and have less side effects. What they all do is restore the neurotransmitter balance so that the patient can think
and feel as he normally would. It restores the mind back to a more normal state of functioning, much like exogenous insulin
might be required to restore a normal state of glucose metabolism in a diabetic. Since we know that some patients are prone
to recurrent neurotransmitter imbalance resulting in frequent depressive symptoms…it makes a lot of sense for these persons to remain on SSRI’s indefinitely(8).
NOTES
-
The quotation from the patient can be found at http://crystal.palace.net~llama/angst/prozac.html.
-
The curve is adapted from Kupfer, D.J. Long-term treatment of depression. J. Clin. Psych. 51, S28–34. The image here is redrawn from http://www.prozac.com/DiseaseInformation/MaximaizingRecovery.jsp.
-
The Zung Tracking Tool can be viewed at https://secure.prozac.com/Main/zung.jsp.
-
From WellCheck® marketing brochure, a Cholestech Service, 2002.
-
On illness identity politics, see Dumit, J. Symptomatic, ill and structurally damned: Notes on liminal creativity and social movements. Paper available at http://symptom.mit.edu.
-
For the Paxil advertisement on imbalance, see http://www.paxil.com/about/nw_bet.html.
-
This notion of “dependent normality” was inspired by Andrew Lakoff’s ethnographic work on normality and mental illness in Argentina.
-
From a Web discussion on “Prozac for everyone.” See http://www.xent.com/aug00/0591.html.
- © American Society for Pharmacology and Experimental Theraputics 2002