For Getting New Drugs into Patients’ Hands, Human Research Accreditation Matters
- Marjorie A. Speers, PhD
Clinical research on human participants is the critical—indeed, rate-limiting—step in the development of therapeutics. A new report issued by the Food and Drug Administration in March, Innovation or Stagnation? Challenge and Opportunity on the Critical Path to New Medical Products (http://www.fda.gov/oc/initiatives/criticalpath/whitepaper.html), identifies both the problems and potential solutions to ensuring that medical science breakthroughs are demonstrated to be safe and effective for patients as quickly and inexpensively as possible. Certainly, the American public has been extraordinarily generous in its support of biomedical research. This generosity, most recently demonstrated in the five-year doubling of the National Institutes of Health budget, rests on the expectation that deeper insights into the mechanisms of health and disease will yield safer, more effective diagnostics, preventatives, and cures. Nevertheless, a series of articles1 in the press has recently explicated the concern that individuals are not volunteering for research studies. Without the participation of the American public, we cannot realize the promise research holds. Indeed, the dearth of human participants is the number one impediment to conducting clinical trials.
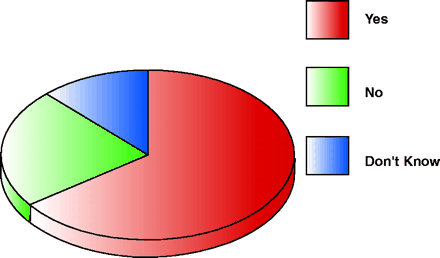
Should we double our research budget?2
The voluntary nature of participation in clinical trials is critically dependent on public trust in the integrity of research organizations and in their commitment to the welfare of human research participants. But today, ethical concerns over the conduct of research involving human participants are squarely in the public eye. Institutional trustworthiness has been compromised in the past few years by widely publicized deaths of research participants. Such events have resulted in the federal government’s suspension of clinical research at some of the nation’s most prestigious academic medical centers, and research organizations now face renewed pressures to comply with federal and state requirements. Clinical investigators must ensure that the research they conduct conforms to the highest ethical standards, not only complying with federal and state overseers, but also assuring the public that the welfare of human research participants is of paramount importance.
The nonprofit founders of the Association for the Accreditation of Human Research Protection Programs (AAHRPP; incorporated 2001) believe that strengthening the quality, integrity, and ethics of clinical research requires an institutional commitment that can best be achieved by accreditation. Accreditation is a time-tested process in the United States, well established in higher education and health care. Accreditation is a voluntary process that ensures quality and stimulates an institutional ethos of excellence by helping organizations conform to a set of standards based on best practices, which are themselves organic and responsive to changes in the disciplines.
AAHRPP employs a voluntary, peer-driven, educational model of accreditation, and was founded upon the belief that ethical soundness and scientific merit in research are inextricably intertwined. AAHRPP was created by seven organizations deeply committed to the ethical conduct of human research, including the Federation of American Societies for Experimental Biology, of which the American Society of Pharmacology and Experimental Therapeutics is a founding member. AAHRPP’s other founders are the Association of American Medical Colleges, the Association of American Universities, the Consortium of Social Science Associations, the National Association of State Universities and Land Grant Colleges, the National Health Council, and Public Responsibility in Medicine and Research (PRIM&R).
Pharmacology and Accreditation
Pharmacology is among the disciplines with great potential for research discoveries that can be translated into medical advances, whether in drug actions, the discovery of new therapies, or the development of new medicinal products. Many pharmacologists conducting basic research are highly motivated by the prospect of getting new drugs into the hands of those who need them. And with the ongoing elucidation of the human genome, many in the research community fore-see a move toward interdisciplinary studies, through which advances will be accelerated by the combined efforts of geneticists, structural biologists and chemists, mathematicians, pharmacologists, and many others.
For pharmacologists who work in university settings, accreditation is particularly important. The inspections that led to the high-profile shutdowns of university research programs in the last several years occurred because of systemic problems with the university’s program for protecting research participants. Although a clinical research study may have been the triggering event, programs were shut down because of significant problems of infrastructure. Those shutdowns thus had a profound influence on all researchers and all research activities at those institutions.
AAHRPP accreditation approaches human research protection from a broad organizational perspective, moving beyond a narrow focus on operations by Institutional Review Boards. AAHRPP standards address the roles and responsibilities of organizations, IRBs, and investigators, examining the sum total of what organizations do to protect research participants.
AAHRPP’s accreditation program is similar to other accreditation programs in terms of process: an organizational self-assessment, an on-site evaluation, and a council of peers that makes accreditation decisions. A helpful comparison might be to the process of animal use and care accreditation by the Association for Assessment and Accreditation of Laboratory Animal Care. Voluntary AAALAC accreditation began nearly forty years ago for research organizations to demonstrate a commitment to the humane use and care of animals in research. Today, more than 650 organizations have achieved AAALAC accreditation. Minimally, these organizations follow applicable law and regulation regarding animal use and care. But more importantly, these organizations see the “value added” by AAALAC accreditation, which serves as an independent, peer-reviewed assessment of their programs, and a demonstration that they go beyond minimal requirements in animal use and care. When controversies surrounding animal use in research arise, AAALAC-accredited organizations are consistently better able to withstand the public scrutiny of their research programs, to justify the need for animal research, and to demonstrate their accountability to the public.
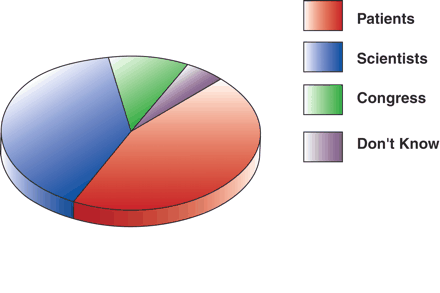
Who should control our research dollars?
Researcher Involvement in Accreditation
The accreditation process provides researchers with a greater voice and an opportunity for greater involvement in their institutions’ human research protection activities, and in institutional research in general. The first step in AAHRPP accreditation is an organizational self-assessment of its human research protection program, measured against AAHRPP standards. Organizations take various approaches to completing the self-assessment, but many appoint committees or task forces to carry it out. The self-assessment is then submitted to AAHRPP along with the application fee, and a site visit is scheduled. Following the site visit, AAHRPP’s Council on Accreditation makes a determination about accreditation status.
The philosophy of AAHRPP’s accreditation embraces two important concepts. First, the peer-based process engages experts in research ethics, IRBs, and various scientific disciplines to compose site visit teams and the Council on Accreditation. In this way, the interests of scientists are represented at each stage of the accreditation process. Second, the accreditation program is designed to be educational—to assist organizations in improving their human research protection programs.
Protection of research participants is a shared responsibility. IRBs have the important and unique responsibility of determining if a research study is ethically justifiable. Once IRBs have approved research, the responsibility for protecting research participants rests with investigators and their research staff. These individuals are responsible for following due procedures in recruiting participants, administering the informed consent process, obtaining voluntary consent, carrying out the methods and interventions of the study, analyzing data, protecting confidentiality, and reporting findings. A weak link in any of these activities both undermines the protection of human research participants and jeopardizes entire research programs. For example, a problem in a clinical trial can lead to institutional changes that affect all investigators, even those far removed from clinical research. Investigators have seen their IRBs enforce stricter requirements for obtaining informed consent and be reluctant to grant exemptions. In other words, a propensity to avoid organizational liability leads to over-interpretation of federal regulations. Investigators thus need to become active in the accreditation process, beginning at the point that their organization initiates the self-assessment. This introspective first step mandates that investigators voice their concerns when they are most likely to be heard and can be addressed.
Participant protection is everyone’s responsibility. Accreditation demonstrates the commitment of institutions, IRBs, and investigators to protecting research participants. Investigators’ involvement in accreditation will assure that participants will be protected, and will also assure that research—and the great promise it holds—moves forward.
Footnotes
- © American Society for Pharmacology and Experimental Theraputics 2004

Marjorie A. Speers, PhD, is Executive Director of the Association for the Accreditation of Human Research Protection Programs. E-mail mspeers{at}aahrpp.org; fax 202-783-1113.



