|
| Article Access Statistics | | | Viewed | 327 | | | Printed | 12 | | | Emailed | 0 | | | PDF Downloaded | 5 | | | Comments | [Add] | | |
|


Click on image for details.
|
|
| |


 |
| Year : 2015 | Volume
: 9
| Issue : 3 | Page : 99-100 |
|
|
|
|
|
LETTER TO THE EDITOR Warm irrigation fluid does not raise the subacromial temperature to harmful levels while using radiofrequency device
Arel Gereli1, Baris Kocaoglu1, Osman Guven2, Metin Turkmen1
1 Department of Orthopedics and Traumatology, Acibadem University Faculty of Medicine, Istanbul, Turkey
2 Acibadem Kadikoy Hospital, Department of Orthopedics and Traumatology Istanbul, Turkey
Correspondence Address:
Baris Kocaoglu
Department of Orthopedic Surgery, Acibadem University Faculty of Medicine, Acibadem Kadikoy Hospital, Tekin Sokak No: 8, 34718 Acibadem, Istanbul
Turkey
 Source of Support: None, Conflict of Interest: None
DOI: 10.4103/0973-6042.161450
 |
|
|
|
| Date of Web Publication | 24-Jul-2015 |
How to cite this article:
Gereli A, Kocaoglu B, Guven O, Turkmen M. Warm irrigation fluid does not raise the subacromial temperature to harmful levels while using radiofrequency device. Int J Shoulder Surg 2015;9:99-100 |
Sir,
Radiofrequency (RF) systems are commonly used for the arthroscopic subacromial decompression. However, there is a concern that the thermal energy generated by the RF probes may have been caused soft tissue damage in the joint if excessive temperatures are reached. [1] Previous studies recommend using room temperature inflowing fluid that differs between 18°C and 24°C. [2] These suggestions bring an important concern, which is hypothermia. Warming of the irrigation fluid may reduce the risk of hypothermia, but the safe limit of the irrigation fluid temperature is unknown. [3] Our hypothesis was that warming the irrigation fluid to actual shoulder temperature would not raise the surrounding temperature to harmful levels while performing bursectomy by RF device.
A prospective Cohort study was performed of 41 consecutive patients underwent arthroscopic subacromial decompression who received irrigation fluid temperature either with 34°C (group 1: Actual shoulder joint temperature, n: 21) or 24°C (group 2: Room temperature, n: 20). Standard posterior and lateral portals were used in all cases. Continuous wave II pump (Arthrex, Naples, Florida) was used for irrigation with a pressure setting of 50 mm Hg and 100 mm Hg flow rate. The RF probe was used intermittently for the subacromial bursectomy process (Arthocare, Knares borough, UK) with a setting 9 and medium level suction. The fiber-optic temperature probe (STB medical probe, Santa Clara, CA, USA) was placed in the subacromial space through an extra anterior portal [Figure 1] and [Figure 2]. Subacromial temperature was observed continuously at 30 s intervals during bursectomy. The total RF usage time was recorded for both groups. Data were analyzed for differences, and any value of P < 0.05 was considered as statistically significant.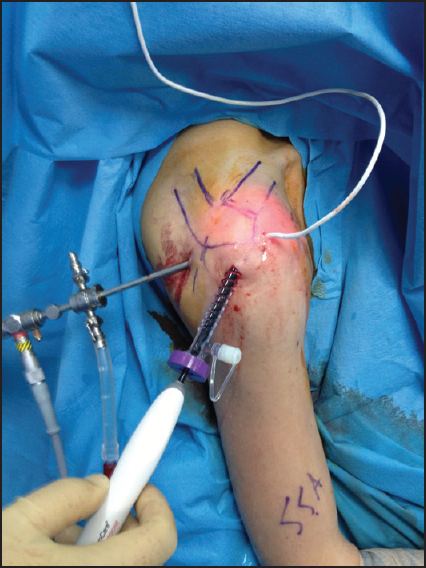 | Figure 1: Standard two arthroscopic portals were used in all cases, and fiber-optic temperature probe was placed in the subacromial bursa through an extra anterior portal
Click here to view |
The mean maximum temperature recorded in the subacromial space while continuous RF usage was 41.8 ± 0.6°C and 31.5 ± 0.6°C at group 1 and 2 respectively (P = 0.001). The peak temperature in the subacromial space was 42.9°C in group 1 and 32.9°C in group 2. There was a positive correlation between the baseline temperature and maximum temperature in both groups (r = 0.794, P = 0.001) but no statistical difference between groups in the case of temperature rise from baseline in subacromial space (P = 0.910). The mean rise in both groups was limited to 7.34 ± 0.7°C. The mean RF usage time was 222 ± 25 s in group 1 and 211 ± 26.4 s in group 2 (P = 0.172). There was no correlation between RF usage time and maximum temperature level in both groups (r = 0.192, P = 0.229).
Temperatures above 45°C can cause nerve and muscle damage, and deemed potentially unsafe for the arthroscopic shoulder surgery. [4] The presented study shows that warming the irrigation fluid at the actual shoulder temperature (34°C) does not raise the subacromial temperature to harmful levels while using bipolar RF device. It can be regarded as an additional measure to prevent hypothermia. A positive correlation between the baseline temperature and maximum temperature in both groups was observed. The higher baseline temperatures appear to correlate with higher subacromial temperatures. However, the mean rise was limited to 7.3°C under standard conditions.
 References References | |  |
| 1. | Lu Y, Bogdanske J, Lopez M, Cole BJ, Markel MD. Effect of simulated shoulder thermal capsulorrhaphy using radiofrequency energy on glenohumeral fluid temperature. Arthroscopy 2005;21:592-6.  |
| 2. | Barker SL, Johnstone AJ, Kumar K. In vivo temperature measurement in the subacromial bursa during arthroscopic subacromial decompression. J Shoulder Elbow Surg 2012; 21:804-7.  |
| 3. | Board TN, Srinivasan MS. The effect of irrigation fluid temperature on core body temperature in arthroscopic shoulder surgery. Arch Orthop Trauma Surg 2008;128:531-3.  |
| 4. | Good CR, Shindle MK, Griffith MH, Wanich T, Warren RF. Effect of radiofrequency energy on glenohumeral fluid temperature during shoulder arthroscopy. J Bone Joint Surg Am 2009;91:429-34.  |
[Figure 1], [Figure 2]
|
|
