|
 
 |
| ORIGINAL ARTICLE |
|
| Year : 2014 | Volume
: 2
| Issue : 1 | Page : 17-20 |
|
A comparison of shear bond strengths of six orthodontic cements
Murat Caglaroglu1, Yusuf Sukurica2, Hakan Gurcan Gurel3, Hakan Keklik1
1 Department of Orthodontics, Faculty of Dentistry, Kirikkale University, Kirikkale, Turkey
2 Private Practice, Konya, Turkey
3 Private Practice, Izmir, Turkey
| Date of Web Publication | 29-Jan-2014 |
Correspondence Address:
Hakan Gurcan Gurel
1386 S N7 D4, Alsancak, Izmir
Turkey
 Source of Support: None, Conflict of Interest: None  | Check |
DOI: 10.4103/2321-3825.125918

Objective: To evaluate the force required to cause debanding when Ultraband-Lok (polyacid-modified composite resin, Reliance Orthodontic Products Inc, Itasca, IL), Optiband (resin-modified glass ionomer, Ormco, West Collins Orange, CA), Meron (glass ionomer, VOCO, Cuxhaven, Germany), Ketac-Cem (glass ionomer, 3M ESPE, St Paul, MN), 3M Multi-cure (resin-modified glass ionomer, 3M Unitek, Monrovia CA), and Transbond Plus (polyacid-modified composite resin, 3M Unitek, Monrovia CA) are used as the luting agents. Materials and Methods: The study sample consisted of 216 intact, caries-free third molars collected from patients attending third molar surgery. To assess the shear bond strength, 216 teeth were randomly divided into six groups of 36 teeth. Stainless steel microetched molar bands were cemented with different cement in each group. To assess shear bond strength, a universal testing machine was used at a crosshead speed of 1 mm/min. Shear bond strength data were analyzed using analysis of variance (ANOVA). Chi-square analysis was used to compare the mode of band failure. Results: No statistically significant difference was found between the groups with regard to shear bond strength (P = 0.919). However, there was a statistically significant difference between the groups with respect to mode of failure (P = 0.004). Conclusion: All evaluated cements yielded comparable shear bond strengths, whereas their mode of failure differed significantly. Keywords: Microetched molar band, orthodontic cement, shear bond strength
How to cite this article:
Caglaroglu M, Sukurica Y, Gurel HG, Keklik H. A comparison of shear bond strengths of six orthodontic cements. J Orthod Res 2014;2:17-20 |
How to cite this URL:
Caglaroglu M, Sukurica Y, Gurel HG, Keklik H. A comparison of shear bond strengths of six orthodontic cements. J Orthod Res [serial online] 2014 [cited 2018 Mar 24];2:17-20. Available from: http://www.jorthodr.org/text.asp?2014/2/1/17/125918 |
| Introduction | |  |
Orthodontic bands are still routinely used in contemporary orthodontics, particularly in areas of high occlusal stress to provide stable attachment for an arch wire, and thus, their retention around the crowns is essential in the successful application of orthodontic forces. [1]
The materials of choice for cementation are commonly the glass ionomer cements (GICs), as these materials adhere to stainless steel and enamel, and also act as a fluoride reservoir helping to prevent decalcification. Conventional GICs have been demonstrated to offer superior retention for stainless steel molar bands in laboratory and clinical trials. [2],[3],[4],[5],[6]
More recently introduced cements include resin-modified GIC (RMGIC) and polyacid-modified composite resin cement. Fluoride release and reuptake occurs with RMGIC in a range similar to that of conventional glass ionomer. [7],[8] Polyacid-modified composite resin cements, are essentially resin composites that slowly release fluoride and have physical properties very similar to resin composite. [9] The results revealed by in vitro studies show that the force values required to remove cemented bands from natural teeth are comparable for RMGIC and GIC, whereas fatigue studies show RMGIC has superior fatigue properties. [10],[11] Studies of the retentive strength of bands cemented with polyacid-modified composite resin cements have demonstrated mixed results, with some investigators finding that polyacid-modified composite resin cements perform equivalent to GIC and RMGIC [11],[12] and others finding lower retentive strength than either RMGIC or GIC. [10]
The aims of this study were to compare the shear bond strength and predominant site of bond failure of microetched orthodontic bands cemented with Ultraband-Lok (polyacid-modified composite resin, Reliance Orthodontic Products Inc, Itasca, IL), Optiband (resin-modified glass ionomer, Ormco, West Collins Orange, CA), Meron (glass ionomer, VOCO, Cuxhaven, Germany), Ketac-Cem (glass ionomer, 3M ESPE, St Paul, MN), 3M Multi-cure (resin-modified glass ionomer, 3M Unitek, Monrovia CA), and Transbond Plus (polyacid-modified composite resin, 3M Unitek, Monrovia CA).
| Materials and Methods | |  |
Two hundred and sixteen caries-free extracted human third molars were collected and cleaned of debris and then stored in distilled water in a refrigerator following decontamination in 0.5% chloramine. The teeth were randomly divided into six groups of 36 teeth, each group comprising 18 maxillary and 18 mandibular third molars. Each tooth was then notched in the apical third with a diamond bur before being mounted to below the amelocemental junction in a block of self-curing acrylic resin with the long axis vertical. The teeth were then cleaned with fluoride-free pumice slurry, rinsed in distilled water, and dried thoroughly in a stream of air. Since bands do not exist for third molars, first permanent molar bands with microetched fitting surfaces (3M Unitek Victory Series, Monrovia, CA) were used. A band was selected and adapted optimally to the crown of each tooth. Thirty-six bands were cemented with each of the six cements. All cements were mixed according to the manufacturers' recommendations at ambient temperature. To standardize specimen preparation, band selection and cementation were performed by one researcher (HK). Once each band had been positioned accurately on the molar crown and pressed firmly into place, excess cement was removed with dry cotton rolls. The light curable cements were cured with a conventional light-curing machine with the duration of exposure recommended by each manufacturer. The specimens were then transferred to a humidor at 37°C for 24 h prior to assessing the shear debonding force using a universal testing machine (Instron, Testometric, Lancheire, UK) with a crosshead speed of 1 mm/min [Table 1].
The specimens were loaded into the jig by two 0.9 mm stainless steel loops which engaged fully under the buccal tube and the lingual cleat of each band. For each specimen, testing proceeded until the band was removed from the tooth. The maximum force (N) recorded during shear-peel debanding was recorded for each specimen and then converted to bond strength values (MPa) using band surface area data provided by the manufacturer. Immediately after the deband testing, specimens were visually assessed to determine the site of cement failure and were classified by the adhesive remnant index (ARI) as originally proposed by Artun and Bergland [13] for bonded brackets and adapted for cemented bands by Millett et al. [10] Scoring was as follows: 0, no cement remains on the tooth surface; 1, less than half of the tooth surface is covered by cement; 2, more than half of the tooth surface is covered by cement; and 3, all of the tooth surface under the band is covered by cement.
After checking the validity of the necessary statistical assumptions (normality and equality of standard deviations in the four groups), one-way analysis of variance (ANOVA) was used to compare mean shear-peel bond strengths of the evaluated cements.
Chi-square analysis was used to compare the mode of band failure.
| Results | |  |
There was no significant difference in mean shear debonding forces of bands bonded with conventional GIC, RMGIC, or modified composite resin (P = 0.919).
There were significant differences between the six cements with regard to the proportion of specimens failing at each of the sites recorded (P = 0.004) [Table 2]. Transbond plus and Ultraband-Lok specimens failed predominantly at the cement/band interface, whereas Ketac-Cem, Meron, Optiband, and 3M Multi-cure specimens failed mostly at the enamel/cement interface [Table 3].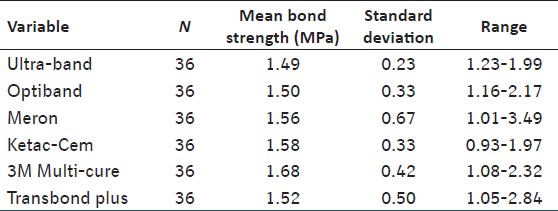 | Table 3: Mean shear bond strength data for each cement used in the study
Click here to view |
| Discussion | |  |
The mean shear bond strength of microetched orthodontic bands cemented with RMGIC, modified composite, and GIC was assessed in the present study. Microetched bands were chosen as these exhibit superior bond strength and a five- to eight-fold lower clinical failure rate compared with untreated bands. [14],[15],[16] Band retention is affected by cement mechanical properties, adhesion at the cement/enamel, and cement/band interfaces and possibly, the influence of repeated mechanical stress on the cement adhesion and cohesion according to previous research. [17],[18],[19],[20]
The mean shear bond strength did not differ significantly between cement groups. Therefore, the present results indicate that conventional GICs are capable of demonstrating a comparable shear bond strength to the other cements evaluated. Millet et al., and Aggarwal et al., also found no significant difference in shear bond strength of bands cemented with RMGIC, modified composite, or conventional GIC confirming the findings of the present study. [11],[12]
In contrast to the results of the present study, Williams et al., reported a higher shear bond strength for modified composite resin cements (Transbond Plus and Ultraband-Lok) compared to conventional GIC evaluated in the short-term (20 min) in their in vitro study. [21] This is in contradiction with the concerns regarding the ability of the light-cured cements, namely Transbond Plus and Ultra Band-Lok, to achieve an acceptable degree of cure, because of the limited area of cement available to the light source. [22] However, their long-term evaluation (6 months) revealed comparable results for the conventional GIC and modified composite resin cement. [21]
Bond failure for bands cemented with Transbond plus and Ultraband-Lok occurred predominantly at the cement/band interface, whereas failure for Ketac-Cem, Meron, Optiband, and 3M Multi-cure specimens occurred mostly at the enamel/cement interface in this study. Millet et al., reported comparable results for the conventional GIC cements in their study. [11] However, 3M Multi-cure failed at the cement/band interface in their study whereas the predominant site of failure for 3M Multi-cure was enamel/cement interface in the present study. Knox et al., demonstrated that the predominant site of failure for GIC (Ketac-Cem), RMGIC (3M Multi-cure), and modified composite (Ultraband-Lok) was cement/band interface. [23] This is in contradiction with the present results except for Ultraband-Lok. In view of the results of the present study, the clean-up time following debanding may be faster clinically where microetched bands are cemented with RMGIC and CGI than with the other cements.
| Conclusions | |  |
There was no significant difference in mean shear debonding forces of bands bonded with conventional GIC, RMGIC, or modified composite resin.
The ARI mode value indicated that bond failure for bands cemented with modified composite resin occurred predominantly at the cement/band interface, whereas failure for GIC and RMGIC specimens occurred mostly at the enamel/cement interface.
| References | |  |
| 1. | Gottlieb EL, Nelson AH, Vogels DS. 1986 JCO study of orthodontic diagnosis and treatment procedures. Part 1. Overall results. J Clin Orthod 1986;20:612-25. 
|
| 2. | Fricker JP, McLachlan MD. Clinical studies on glass ionomer cements. Part 2. A two year clinical study comparing glass ionomer cement with zinc phosphate cement. Aust Orthod J 1987;10:12-4. 
|
| 3. | Norris DS, McInnes-Ledoux P, Schwaninger B. Weinberg R. Retention of orthodontic bands with new fluoridereleasing cements. Am J Orthod 1986;89:206-11. 
|
| 4. | Mizrahi E. Glass ionomer cements in orthodontics--an update. Am J Orthod Dentofacial Orthop 1988;93:505-7. 
[PUBMED] |
| 5. | Stirrups DR. A comparative clinical trial of a glass ionomer and a zinc phosphate cement for securing orthodontic bands. Br J Orthod 1991;18:15-20. 
[PUBMED] |
| 6. | Durning P, McCabe JF. Gordon PH. A laboratory investigation into cements used to retain orthodontic bands. Br J Orthod 1994;21:27-32. 
|
| 7. | O′Brien WJ, editor. Dental Materials and Their Selection. 3 rd ed. Carol Stream: Quintessence; 2002: 260. 
|
| 8. | Eliades G. Chemical and biological properties of glass-ionomer cements. In: Davidson CL, Mjor IA, editors. Advances in Glass-Ionomer Cements. Carol Stream: Quintessence; 1999. p. 85-101. 
|
| 9. | Craig RG, Powers JM, Wataha JC. Dental Materials: Properties and Manipulation. St Louis: CV Mosby Co; 2000:57-78. 
|
| 10. | Millett DT, Duff S, Morrison L, Cummings A, Gilmour WH. In vitro comparison of orthodontic band cements. Am J Orthod Dentofacial Orthop 2003;123:15-20. 
[PUBMED] |
| 11. | Millett DT, Cummings A, Letters S, Roger E, Love J. Resinmodified glass ionomer, modified composite or conventional glass ionomer for band cementation?-an in vitro evaluation. Eur J Orthod 2003;25:609-14. 
[PUBMED] |
| 12. | Aggarwal M, Foley TF, Rix D. A comparison of shear-peel band strengths of 5 orthodontic cements. Angle Orthod 2000;70:308-16. 
[PUBMED] |
| 13. | Artun J, Bergland S. Clinical trials with crystal growth conditioning as an alternative to acid-etch enamel pretreatment. Am J Orthod 1984;85:333-40. 
[PUBMED] |
| 14. | Millett DT, McCabe JF, Bennett TG, Carter NE, Gordon PH. The effect of sandblasting on the retention of first molar orthodontic bands cemented with glass ionomer cement. Br J Orthod 1995;22:161-9. 
[PUBMED] |
| 15. | Mennemeyer VA, Neuman P, Powers JM. Bonding of hybrid ionomers and resin cements to modified orthodontic band materials. Am J Orthod Dentofacial Orthop 1999;115:143-7. 
[PUBMED] |
| 16. | Hodges SJ, Gilthorpe MS, Hunt NP. The effect of microetching on the retention of orthodontic molar bands: A clinical trial. Eur J Orthod 2001;23:91-7. 
[PUBMED] |
| 17. | Williams JD, Swartz ML, Phillips RW. Retention of orthodontic bands as influenced by the cementing media. Angle Orthod 1965;35:278-85. 
[PUBMED] |
| 18. | Bills RC, Yates JL, McKnight JP. Retention of stainless steel bands cemented with four dental cements. J Pedod 1980;4:273-86. 
|
| 19. | Hotz P, McLean JW, Sced I, Wilson AD. The bonding of glass ionomer cements to metal and tooth substrate. Br Dent J 1977;142:41-7. 
[PUBMED] |
| 20. | Abu Kasim NH, Millett DT, McCabe JF. The ball mill as a means of investigating the mechanical failure of dental materials. J Dent 1996;24:117-24. 
[PUBMED] |
| 21. | Williams PH, Sherriff M, Ireland AJ. An investigation into the use of two polyacid-modified composite resins (compomers) and a resin-modified glass poly (alkenoate) cement used to retain orthodontic bands. Eur J Orthod 2005;27:245-51. 
[PUBMED] |
| 22. | Sargison AE, McCabe JF, Gordon PH. An ex vivo study of self-, light-, and dual-cured composites for orthodontic bonding. Br J Orthod 1995;22:319-23. 
[PUBMED] |
| 23. | Knox J, Chye KY, Durning P. An ex vivo evaluation of resin-modified glass polyalkenoates and polyacid-modified composite resins as orthodontic band cements. J Orthod 2004;31:323-8. 
[PUBMED] |
[Table 1], [Table 2], [Table 3]
|