|
 
 |
| ORIGINAL ARTICLE |
|
| Year : 2015 | Volume
: 10
| Issue : 3 | Page : 81-86 |
|
Clinical interactions of honey with antidiabetic drugs among some Sudanese diabetic patients in Khartoum, 2013
Aimun A E Ahmed1, Wadeaa A Fadl-Almawla2, Amina A Gasm-El-Bari2, Zuheir Osman3
1 Department of Pharmacology, Faculty of Pharmacy, Omdurman Islamic University, Omdurman, Sudan
2 Department of Pharmacology, Faculty of Pharmacy, International University of Africa, Khartoum, Sudan
3 Department of Pharmaceutics, Faculty of Pharmacy, University of Khartoum, Khartoum, Sudan
| Date of Web Publication | 21-Oct-2015 |
Correspondence Address:
Aimun A E Ahmed
Department of Pharmacology, Faculty of Pharmacy, Omdurman Islamic University, P. O. Box: 382, Omdurman
Sudan
  | Check |
DOI: 10.4103/1858-5000.167864 
Background: The aim of the study was to assess the possible interactions of honey with anti-diabetic drugs used by the Sudanese diabetic patients attending two main hospitals in Khartoum, Sudan. Methods: The study was two month, cross-sectional, hospital-based study, during the period from April to May, 2013. Results: 260 of diabetic patients were chosen and only 68 were enrolled in the study, 32 (47.1%) were male and 36 (52.9%) females, the majority were elderly 32(47%), the patients were from different tribes and different areas. The majority of the patients were from Khartoum 24 (35.2%) and central Sudan 23 (33.8%), 51 (75%)of the patients were clinically diagnosed with type 2 diabetes mellitus, Hypertension as complication was found in 39.7% of the patients whilst 39.7% were without complications. Conclusions: The use of the honey concurrently with anti-diabetic drugs was with significant positive effect. Our findings revealed that, the illiterate and university patients' represent the majority regarding the honey utilization. The majority of respondents use honey according to their own knowledge and did not inform her/his doctors. Keywords: Diabetic, drugs, honey, hypoglycemic, interactions, Sudanese
How to cite this article:
Ahmed AA, Fadl-Almawla WA, Gasm-El-Bari AA, Osman Z. Clinical interactions of honey with antidiabetic drugs among some Sudanese diabetic patients in Khartoum, 2013. Sudan Med Monit 2015;10:81-6 |
How to cite this URL:
Ahmed AA, Fadl-Almawla WA, Gasm-El-Bari AA, Osman Z. Clinical interactions of honey with antidiabetic drugs among some Sudanese diabetic patients in Khartoum, 2013. Sudan Med Monit [serial online] 2015 [cited 2018 Sep 5];10:81-6. Available from: http://www.sudanmedicalmonitor.org/text.asp?2015/10/3/81/167864 |
| Introduction | |  |
Diabetes mellitus (DM) is a metabolic disorder resulting from a defect in insulin secretion, action, or both. Insulin deficiency in turn leads to chronic hyperglycemia. [1]
As the disease progresses, tissue or vascular damage will occur leading to severe diabetic complications such as retinopathy, neuropathy, nephropathy, ischemic heart disease, stroke and peripheral vascular disease, and diminished quality of life. [2],[3]
Diabetes is the most common endocrine disorder by the year 2010. It is estimated that more than 200 million people worldwide will have DM and 300 million will subsequently have the disease by 2025. [1] The majority of DM populations will emerge from developing countries that often had a poor glycemic control, with a high prevalence of acute and chronic complications, and a low quality of life. [2]
Several types of Oral hypoglacemic agents were avilable and used to lower the high Blood glucose level such as sulfonylureas, thiazolidinedione, biguanide, and acarbose. [3]
The American Diabetes Association estimated the national costs of diabetes in the USA for the year 2002 to be $USA 132 billion, increasing to $USA 192 billion in 2020. [4]
Elamin et al., in 1992, stated that, in Sudan, due to limited resources, most of the patients (51%) had reduced or abandoned insulin therapy due to nonavailability or no affordability of this drug. Most patients did not receive satisfactory diabetes care and oriented educations, leading to a lower rate of clinic attendance (55%) and had poor dietary knowledge (78.5%). [5]
In Sudan, few drugs available to manage the DM are not readily affordable to the poor people [6] whom represent the majority of the Sudanese people. [7]
The most recent data from a small-scale study conducted in 1996 indicated 3.4% of the prevalence in morbidity and mortality of DM in Sudan. [8] While the recent report estimates the diabetes population at around 1 million (95%) among type 2 diabetes patients. [9]
Many factors governed the DM control among Sudanese such as economic problems, [7],[8] educational level, [10] particularly the knowledge regarding diabetes.
Honey is a natural substance produced by bees from nectar. The composition of honey is influenced by a number of factors such as geographical origin, botanical sources of nectar, environmental and climatic conditions as well as processing techniques. [11]
Therefore, research on the desired pharmacological effects and possible unwanted side effects or toxicity is required despite the availability of various classes of antidiabetic agents. [12]
Honey was used widely by Sudanese diabetic patients due to cultural beliefs about their safety and its magic healing power reported by the prophet.
This study aimed to assess the possible interactions exist with the concurrent use of honey with conventional available hypoglycemic agents used by Sudanese diabetic patients in two main teaching hospitals in the capital of the Sudan during 2013 summer.
| Materials and methods | |  |
Ethical considerations
The study was approved by the National Committee represented as The Research Department, Ministry of Health, Khartoum state, in the form of Ethical Clearance. Besides, patient informed consent was filled by all participant patients or their co-patients in individualized patterns.
Study design
A cross-sectional, hospital-based concurrent survey was conducted on diabetic patients in two major hospitals in the capital of Sudan. Hospitals were selected according to their capabilities to fit our study population needs, namely:
- Khartoum Teaching Hospital, particularly its referring clinic unit
- Al-Ribat Teaching Hospital with its special units for diabetic and diabetes education center.
Study population
Type 1 and type 2 diabetic patients attending the outpatient clinic in the two selected hospitals were enrolled in the study.
All diabetic patients taking honey were actively included in the study while those whom did not meet our criteria were excluded.
Sample size
The simplest formula of sample size determination (N = PQZ 2 /d 2 ) was used to estimate our sample size (N = 384).
Where N = sample size, P = prevalence factor, Q = 1−p, Z = constant 95% occurred 1.96, and d = desired margin.
Data collection
Patients were interviewed through a predesigned questionnaire that contains items that are directly related to diabetes and the concurrent use of honey with antidiabetic drugs.
Patients were asked about their personal information and then with regards to their diabetes condition (type, duration, date of diagnosis, and type of medications used for the treatment of DM).
They were asked further questions regarding the honey used, such as honey source, insist to use it, frequency of use, who prescribed it, experience of any effect(s), and if he/she had informed his/her doctor.
Data analysis
Statistical evaluation was performed with Statistical Package for Social Science (SPSS) computer program version 16 release 16.0.0 (September 13, 2007), copyright (c) SPSS Inc., USA. Data were analyzed by means of the Chi-square test to compare the mean differences for various results. The differences were considered to be significant at P ≤ 0.05.
| Results | |  |
Patients' characteristics
From a total of 384 data collection form, only 260 were filled and 68 of the patients met our criteria and enrolled in the study.
The gender distribution of the study population showed that 32 (47.1%) were males and 36 (52.9%) were females. The age of the subjects enrolled into the study ranged from 16 years to >60 years old. The educational level of the subjects ranged from noneducated, completing less than high school to completion of a graduate school degree. In this category, 32.3% of the study patients were illiterates (n = 22), while the university represented 23 (33.8%). The residence distribution of the study population showed that more than 50% lives in the capital and central of the Sudan and no participant came from the South country part as seen in [Table 1].
Disease status among the participants
39.7% of the participants have no complications with DM and the same proportion have hypertension as shown in [Figure 1].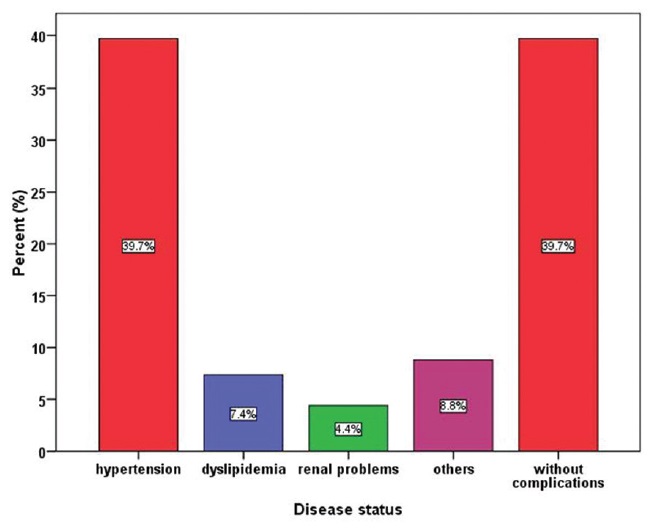 | Figure 1: Patterns of the disease status associated with diabetes among the participants
Click here to view |
Depending on the gender factor, 75% (n = 51) of the respondents were diagnosed with type 2 DM, whereas type 1 DM represents 25% (n = 17).
Regarding the medication used by patient, sulfonylurea represents 36.8% (n = 25), and use by male represents 31.3% (n = 10) while female use appears to be 41.7% (n = 15) as shown in [Table 2].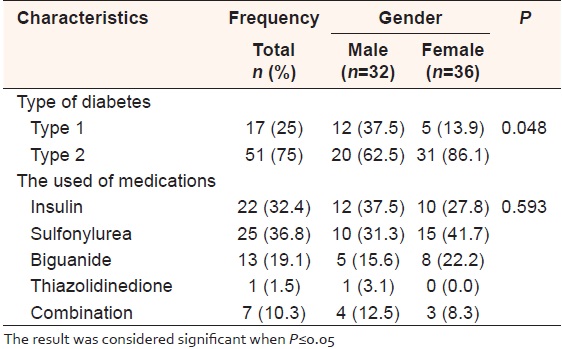 | Table 2: Patterns of the diabetes type and the drug used based on the gender type (n=68)
Click here to view |
Answer of respondents to questions regarding the honey use
The survey revealed that different honey sources were shown in [Figure 2], depending on patient education level, 66.2% of the patients obtained the honey from the trusted source, while 27.9% of them obtained the honey directly from the market [Figure 2], besides, 68.2% of the university respondents and 72.7% of the illiterates believed that honey was safe and insisted to use it.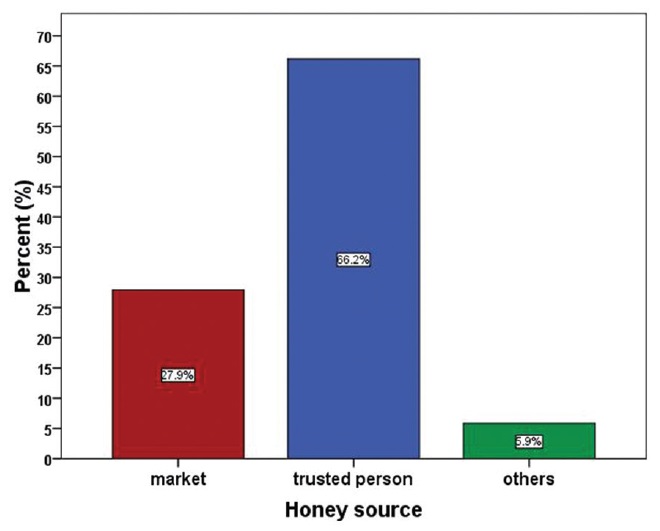 | Figure 2: Summary of the respondents answer to the question regarding the honey source
Click here to view |
Moreover, majority of the respondents used honey based on their self-knowledge and did not inform their doctors, while the majority of the honey users were insisted and planed to use honey again, these findings are shown in [Table 3].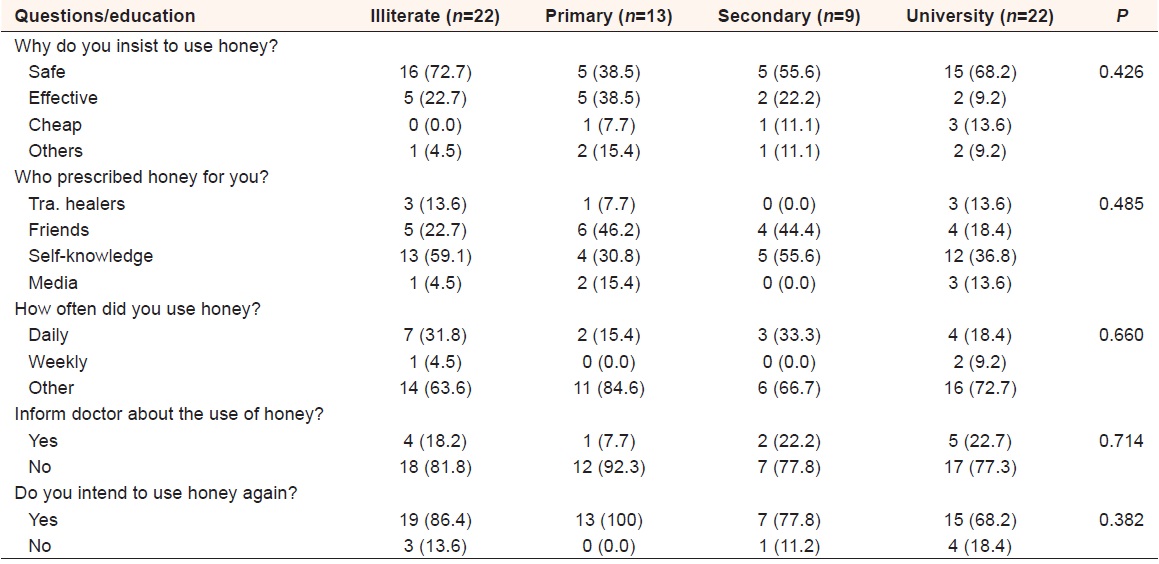 | Table 3: Summary of the respondents answers to the questions regarding the honey use based on their educational level (n=68), missed (n=2)
Click here to view |
The clinical interaction patterns of honey with antidiabetic agents
Half of the participents reported that, Honey was effective in lowering the Blood glucose when used concomitently with antidiabetic agnets, whilst the rest opinion regarding honey effectivness, either null or not sure [Figure 3].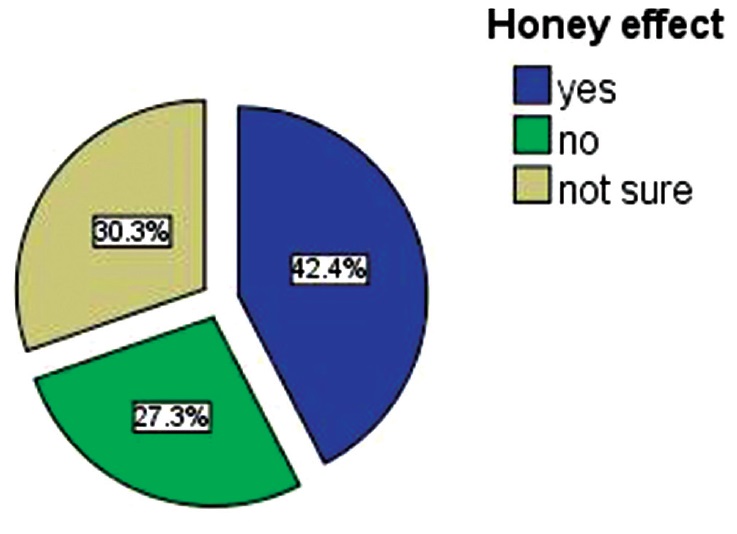 | Figure 3: Participants opinions regarding the effectiveness of the honey use
Click here to view |
| Discussion | |  |
Recently, there was a renewed interest in the use of natural products, including honey, in the treatment of diabetes. [13]
From the suggested sample size, only 260 patients returned and only 68 (26.2%) met the study criteria and enrolled into the study, this was due to the lack of some patients' co-operation.
The study characterization showed no significant variation in gender, residence, and educational level among the participants, except in the age that vary significantly (P = 0.047), indicating the proper sample selection with minimum observers bias which reflects the true phenomenon distribution among the study population.
Because the study was conducted in Khartoum Teaching Hospital and Al-Ribat Teaching Hospital, most of the patients were from Khartoum and central Sudan.
This survey reported that the DM complications among the participants were mainly; hypertension, or without complications, also the DM type was found to be type 2 and the commonest hypoglycemic agent used was sulfonylurea, this may be due its affordability.
Our findings revealed that there was a restriction of the honey use among the participants, while the illiterate and university patients' represent the majority regarding the honey utilization.
The majority of participants were insisted to use honey, because, they think it is safe regardless its efficiency and they use honey irregularly.
The majority of respondents were catalyzed to be honey user according to their own knowledge. This may draw attention to the importance of health education to the communities.
Although, the majority of participants obtained honey from trusted person, they believed that honey was safe as a sweetening agent. While others obtain it directly from the market and did not care about its originality, which was a determining factor for safety.
In spite of half of the diabetic patients whom used honey irregularly by their own self-knowledge as it mentioned in prophetic medicine, recent findings indicated that honey improves glycemic control and exerts hypoglycemic effect in nondiabetic, alloxan, and streptozotocin-induced diabetic rats. [11],[12]
Other study showed that the combination of antidiabetic drugs with honey improves glycemic control in diabetic rats, [14] while in humans, honey supplementation reduces hyperglycemia. [15],[16]
All honey users did not inform her/his doctors, reasoning that some patients may be worried regarding the negative attitude of doctors toward honey and will be insisted to use it again, this may be due to their high trust of their self-knowledge that was based on their culture and religion. The diabetes health care providers observed patients with practices that adversely affect their condition management. [17]
Although different hypoglycemic agents were used at the same time with honey, half of the patients reported positive effect for the honey, which can be taken as an evident to support the cultural information and practices, whereas others either did not observe or not sure about the honey effect.
| Conclusion and recommendations | |  |
In Sudan, based on cultural and religious reasons, honey was used by DM patient at the same time with antidiabetic drugs to manage the glucose level and to decrease the complications.
Doctors should be aware about the use of honey, as it may affect the outcome and the management of their disease.
We recommended future deep clinical studies that enlisted a large sample size for investigating the potential role of honey in the management of DM and their clinical interactions with antidiabetic drugs.
Consumption of limited amounts of honey was believed to be safe and help to control diabetes, also compensate their intake of vitamins and nutrients such as B1, B6, B12, C, and E, as well as Biotin, but patients had to make sure that it was pure, raw, and organic honey and not adulterated by starch, glucose, or even malt.
It was important to consult a doctor adopting this practice.
Acknowledgment
Grateful thanks was expressed to Khartoum teaching hospital and Al-Ribat Teaching Hospital staff.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| References | |  |
| 1. | Amos AF, McCarty DJ, Zimmet P. The rising global burden of diabetes and its complications: Estimates and projections to the year 2010. Diabet Med 1997;14 Suppl 5:S1-85.  |
| 2. | Shaw JE, Sicree RA, Zimmet PZ. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res Clin Pract 2010;87:4-14.  |
| 3. | Al-Mubaslat A. Type 2 diabetes mellitus cause, symptom, treatment, diagnosis. Clin Diabetes 2013;61:4905-13.  |
| 4. | Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: Estimates for the year 2000 and projections for 2030. Diabetes Care 2004;27:1047-53.  |
| 5. | Elamin A, Altahir H, Ismail B, Tuvemo T. Clinical pattern of childhood type 1 (insulin-dependent) diabetes mellitus in the Sudan. Diabetologia 1992;35:645-8.  |
| 6. | Abdelgadir M, Elbagir M, Eltom A, Eltom M, Berne C. Factors affecting perinatal morbidity and mortality in pregnancies complicated by diabetes mellitus in Sudan. Diabetes Res Clin Pract 2003;60:41-7.  |
| 7. | Ahmed A. Diabetes mellitus in Sudan: Size of proplem and possibilties of efficient care. Pract Diabetes Int 2001;18:7-342.  |
| 8. | Ahmed AM , Ahmed NH, Abdalla ME. Pattern of hospital mortality among diabetic patients in Sudan. Pract Diabetes Int 2000;90:3-41.  |
| 9. | Elbagir MN, Eltom MA, Elmahadi EM, Kadam IM, Berne C. A population-based study of the prevalence of diabetes and impaired glucose tolerance in adults in northern Sudan. Diabetes Care 1996;19:1126-8.  |
| 10. | Ahmed A, Ahmed N. Diabetes mellitus in Sudan: the size of the problem and the possibilities of efficient care. Pract Diabetes Int 2001;18:324-7.  |
| 11. | Chepulis L, Starkey N. The long-term effects of feeding honey compared with sucrose and a sugar-free diet on weight gain, lipid profiles, and DEXA measurements in rats. J Food Sci 2008;73:H1-7.  |
| 12. | Erejuwa OO, Sulaiman SA, Wahab MS. Fructose might contribute to the hypoglycemic effect of honey. Molecules 2012;17:1900-15.  |
| 13. | Bogdanov S, Jurendic T, Sieber R, Gallmann P. Honey for nutrition and health: A review. J Am Coll Nutr 2008;27:677-89.  |
| 14. | Erejuwa OO, Gurtu S, Sulaiman SA, Ab Wahab MS, Sirajudeen KN, Salleh MS. Hypoglycemic and antioxidant effects of honey supplementation in streptozotocin-induced diabetic rats. Int J Vitam Nutr Res 2010;80:74-82.  |
| 15. | Erejuwa OO, Sulaiman SA, Wahab MS, Sirajudeen KN, Salleh MS, Gurtu S. Glibenclamide or metformin combined with honey improves glycemic control in streptozotocin-induced diabetic rats. Int J Biol Sci 2011;7:244-52.  |
| 16. | Yaghoobi N, Al-Waili N, Ghayour-Mobarhan M, Parizadeh SM, Abasalti Z, Yaghoobi Z, et al. Natural honey and cardiovascular risk factors; effects on blood glucose, cholesterol, triacylglycerole, CRP, and body weight compared with sucrose. Scientific World Journal 2008;8:463-9.  |
| 17. | Ahmed A, Ahmed NH. Diabetes mellitus in Sudan: The size of the problem and the possibilities of efficient care. Pract Diabetes Int 2001;18:211-8.  |
[Figure 1], [Figure 2], [Figure 3]
[Table 1], [Table 2], [Table 3]
|