|
 
 |
| CASE REPORT |
|
| Year : 2015 | Volume
: 3
| Issue : 1 | Page : 65-69 |
|
Bone-anchored maxillary protraction followed by fixed appliances in skeletal Class III malocclusion: A report of two cases
Emine Kaygisiz1, Erdal Bozkaya1, Sema Yuksel1, Erkan Erkmen2, Mustafa Sancar Atac2
1 Department of Orthodontics, Faculty of Dentistry, Gazi University, Ankara, Turkey
2 Department of Oral and Maxillofacial Surgery, Faculty of Dentistry, Gazi University, Ankara, Turkey
| Date of Web Publication | 29-Dec-2014 |
Correspondence Address:
Emine Kaygisiz
Department of Orthodontics, Faculty of Dentistry, Gazi University, 8, Cad. 82. Sok No: 4, Emek, Ankara 06510
Turkey
 Source of Support: None, Conflict of Interest: None  | Check |
DOI: 10.4103/2321-3825.146362

Maxillary protraction is recommended for patients with skeletal Class III malocclusion diagnosed with maxillary deficiency. The major goal of the protraction is to correct maxillary discrepancy with a skeletal alteration rather than dental movements. However, loss of the dental anchorage has been reported beside the skeletal effects with facemask therapy using tooth-borne anchorage. The use of miniscrews and miniplates became popular as an anchorage instead of conventional tooth-borne appliances. Studies evaluating the second-phase treatment results and stability of bone-anchored maxillary protraction are needed in literature. This case report presents the treatment of 11 and 12-year-old two boys with Class III malocclusion due to maxillary deficiency. Both cases were treated with fixed appliances subsequent to maxillary protraction with miniplates. Maxillary skeletal effects were increased, and undesired dentoalveolar effects were reduced by the facemask therapy with skeletal anchorage. The occlusion and the facial profile were effectively improved, with good stability after fixed appliances. Keywords: Bone-anchor, facemask, maxillary protraction, miniplate, second-phase treatment
How to cite this article:
Kaygisiz E, Bozkaya E, Yuksel S, Erkmen E, Atac MS. Bone-anchored maxillary protraction followed by fixed appliances in skeletal Class III malocclusion: A report of two cases. J Orthod Res 2015;3:65-9 |
How to cite this URL:
Kaygisiz E, Bozkaya E, Yuksel S, Erkmen E, Atac MS. Bone-anchored maxillary protraction followed by fixed appliances in skeletal Class III malocclusion: A report of two cases. J Orthod Res [serial online] 2015 [cited 2018 Sep 6];3:65-9. Available from: http://www.jorthodr.org/text.asp?2015/3/1/65/146362 |
| Introduction | |  |
Tooth-borne anchorage devices have been used commonly to transfer the protraction force to the maxilla in patients with skeletal Class III malocclusion due to maxillary retrusion. These methods cause tooth movements beside the skeletal effects. [1],[2],[3] However, the major aim of the protraction is to correct maxillary discrepancy with a skeletal alteration rather than the teeth. Skeletal anchorage became popular to transfer orthopedic forces directly to the maxilla. [4],[5],[6] Studies evaluating the results of the second-phase treatment and stability of bone-anchored maxillary protraction are needed in literature. This case report presents the outcomes of maxillary protraction with miniplates and second-phase treatment in two cases.
| Case Reports | |  |
In this report, two maxillary deficiency cases were treated with Delaire-type facemask with miniplates, and protraction was followed by fixed therapy. Dentoskeletal effects of bone-anchored maxillary protraction and overall treatment changes including fixed therapy were evaluated in both cases. This study was approved by the Ethics Committee of the University (824-02/9-8/5).
Case I
The patient, an 11-year-old boy, presented anterior crossbite, retrusive nasomaxillary area and upper lip [Figure 1]. His skeletal age was 11 year and 6 months. The cephalogram showed skeletal Class III malocclusion due to maxillary deficiency and mandibular prognatism, and an optimum mandibular plane angle [Table 1].
Case II
The patient, a 12-year-old boy, presented anterior cross bite, retrusive nasomaxillary area and upper lip, impacted right maxillary canine [Figure 2]. His skeletal age was 11 years. The cephalogram showed a skeletal Class III malocclusion due to maxillary deficiency, and an increased mandibular plane angle [Table 2].
In the first case, proper over jet was established within 19 months, and 8 months in the second one. After protraction, the first case was treated without extraction for 9 months for final detailing of occlusion, and the second one with extraction of maxillary and mandibular first premolars for 2 years. Both patients didn't use facemask during fixed appliances.
Surgical and Orthopaedic Protocol of Bone-Anchored Maxillary Protraction
I-shaped titanium miniplates (Tasarύmmed, Istanbul, Turkey) were inserted both zygomatic buttresses of the maxilla, and stabilized with 3-titanium screws (diameter, 2 mm; length, 5 mm) per side [Figure 3]. The straight arm of the miniplate was curved for elastic traction and exposed to the buccal side of first premolars. One week later from insertion of miniplates, the patients were instructed to wear a facemask all day and night except meals. An intraoral plate on the lower arch with a minimum thickness sufficient to open the bite to an edge-to-edge incisal position was used. The force was started with 150 g from the miniplates by elastics per side and increased to 250 g after 1 month.
Lateral cephalometric and hand-wrist radiographs were taken before treatment (T1), after a proper over jet was obtained (T2), and at the end of the fixed therapy (T3).
Total superimpositions were made on the best fit of the anterior cranial base. Local superimpositions were made on the best fit of the palatal structures for the maxilla, and on the best fit of the posterior border of the symphysis and inferior border of the mandible. For each superimposition, the pre-treatment tracing T-W line was used as the horizontal reference line. A vertical line perpendicular to T-W at point T was used as a vertical reference plane.
Treatment Results
3 and 2 mm forward movements of A-point were observed in Case I and II, respectively [Figure 4] and [Figure 5]. Slight anterior rotations of the maxilla and advancements of orbitale and pterygomaxillare were observed in both cases.
While intermaxillary relationship was improved by mainly maxillary protraction, restraining effects on mandibular growth were also recorded in both cases. Mandibular plane angle didn't change in Case I, however increased slightly in Case II. Overjet improved to 4 mm in Case I and 3.5 mm in Case II. Protrusion of the maxillary incisors was observed in Case I, however retrusion of the maxillary incisors was observed in Case II. Mandibular incisors were retruded in both cases [Figure 6] and [Figure 7]. Slight mesialization of maxillary molars was observed in both cases.
In the second-phase of treatment, forward growth of the maxilla and posterior rotation of mandible and retrusion of maxillary incisors were observed in both cases. The position of pterygomaxillare and orbitale were maintained [Figure 8] and [Figure 9].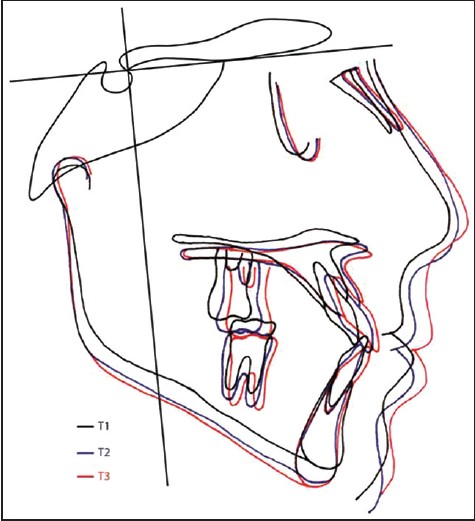 | Figure 4: Preprotraction, postprotraction and posttreatment cephalometric superimposed tracings of Case I
Click here to view |
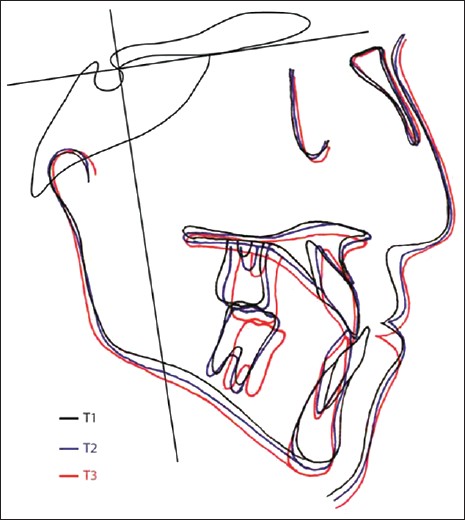 | Figure 5: Preprotraction, postprotraction and posttreatment cephalometric superimposed tracings of Case II
Click here to view |
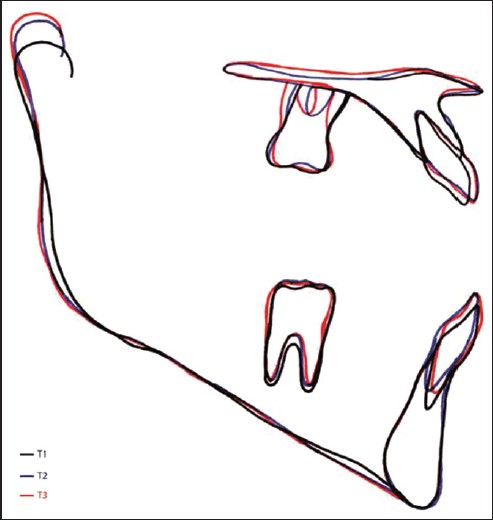 | Figure 6: Local preprotraction, postprotraction and posttreatment cephalometric superimposed tracings of Case I
Click here to view |
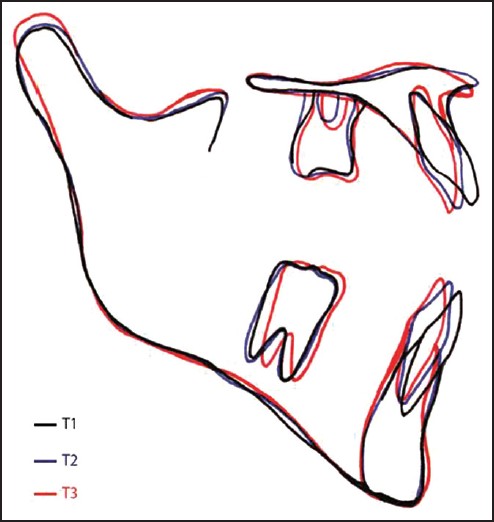 | Figure 7: Local preprotraction, postprotraction and posttreatment cephalometric superimposed tracings of Case II
Click here to view |
| Discussion | |  |
Titanium miniplates had become the most popular anchorage device for facemask therapies. Lateral nasal walls and zygomatic buttresses of the maxilla were both used for miniplate insertion in previous studies. [7],[8] However, there was a denser bone in the zygomatic buttress area for miniplate insertion. [9] Hence, miniplates in the zygomatic buttresses were preferred for skeletal anchorage.
In both cases, maxillary advancement wasn't limited to the alveolar bone but extended up to the levels of the pterygomaxillary fissure, and orbital ridge as well. This finding suggested that whole maxilla moved forward by protraction. Previous bone-anchored facemask studies reported higher amounts of maxillary advancement. [5],[6],[7],[10] This difference might be due to the lower protraction force and relatively older ages, as the ages of both patients were >10 years. During the second-phase treatment, the less amount of protraction was observed in both cases. This result could be attributed to the return of previously existing growth pattern. Similar results have been reported during the follow-up of conventional facemask therapy. [1],[2],[10]
Vertical changes were better controlled with bone-anchored maxillary protraction which was in concomitant with bone-anchored facemask studies. [1],[4],[5],[6] In contrast with this, some authors reported significant posterior rotation of mandible and decrease in SNB angle by the conventional facemask treatment. This difference may relate to significant anterior rotation of the maxilla. [2],[9],[10] During the second-phase, posterior rotation of mandible was observed due to fixed appliances and individual growth patterns in both cases.
Changes in the maxilla and the mandible resulted with increases in ANB angle in both cases. This result is in accordance with the results of previous studies which aimed to correct the skeletal Class III relation. [1],[2],[5],[6],[7] During second-period, maxilla and mandible showed harmonious growth, maintaining an ANB difference of 1.5° and 2° in Case I and II, respectively.
Proclination of maxillary incisors and mesialization of maxillary molars are undesirable effects of the conventional facemask therapies. [1],[2],[3] In Case II, maxillary incisors were retruded in accordance with bone-anchored facemask studies. [2],[3],[5],[7] However, in Case I proclination of maxillary incisors was observed which might be due to the prolonged use of facemask appliance. Mandibular incisors were retruded in both cases due to the chincap effect of facemask. This finding is in concomitant with facemask studies with and without skeletal anchorage. [2],[3],[5],[10]
Favorable results were achieved with bone-anchored maxillary protraction although the lower protraction force in relatively older patients. After the second-phase treatment, morphologically and functionally stable results were observed. Skeletal Class III malocclusions might be treated with bone-anchored maxillary protraction combined with fixed appliances to reduce treatment time.
| References | |  |
| 1. | Franchi L, Baccetti T, McNamara JA. Postpubertal assessment of treatment timing for maxillary expansion and protraction therapy followed by fixed appliances. Am J Orthod Dentofacial Orthop 2004;126:555-68.  |
| 2. | Chong YH, Ive JC, Artun J. Changes following the use of protraction headgear for early correction of class III malocclusion. Angle Orthod 1996;66:351-62.  |
| 3. | Seehra J, Fleming PS, Mandall N, Dibiase AT. A comparison of two different techniques for early correction of class III malocclusion. Angle Orthod 2012;82:96-101.  |
| 4. | Yan X, He W, Lin T, Liu J, Bai X, Yan G, et al. Three-dimensional finite element analysis of the craniomaxillary complex during maxillary protraction with bone anchorage vs conventional dental anchorage. Am J Orthod Dentofacial Orthop 2013;143:197-205.  |
| 5. | Sar C, Arman-Özçýrpýcý A, Uçkan S, Yazýcý AC. Comparative evaluation of maxillary protraction with or without skeletal anchorage. Am J Orthod Dentofacial Orthop 2011;139:636-49.  |
| 6. | Sar C, Sahinoðlu Z, Özçirpici AA, Uçkan S. Dentofacial effects of skeletal anchored treatment modalities for the correction of maxillary retrognathia. Am J Orthod Dentofacial Orthop 2014;145:41-54.  |
| 7. | Kircelli BH, Pektaº ZO, Uçkan S. Orthopedic protraction with skeletal anchorage in a patient with maxillary hypoplasia and hypodontia. Angle Orthod 2006;76:156-63.  |
| 8. | Coscia G, Addabbo F, Peluso V, D'Ambrosio E. Use of intermaxillary forces in early treatment of maxillary deficient class III patients: Results of a case series. J Craniomaxillofac Surg 2012;40:e350-4.  |
| 9. | Melsen B, Verna C. Miniscrew implants: The Aarhus anchorage system. Semin Orthod 2005;11:24-31.  |
| 10. | Kircelli BH, Pektas ZO. Midfacial protraction with skeletally anchored face mask therapy: A novel approach and preliminary results. Am J Orthod Dentofacial Orthop 2008;133:440-9.  |
[Figure 1], [Figure 2], [Figure 3], [Figure 4], [Figure 5], [Figure 6], [Figure 7], [Figure 8], [Figure 9]
[Table 1], [Table 2]
|